What Is Medicare: Medicare is the federal health insurance program for people who are 65 years of age or older, or certain younger people with disabilities.
U.S. citizens and legal residents.
Legal residents are required to live in the United States for at least 5 consecutive years, including the 5 years just before applying for Medicare.
The following requirements must also be met:
65 Years or older Younger than 65 years old with a qualifying disability Any age with a diagnosis of end-stage renal disease (ESRD) or amyotrophic lateral sclerosis (ALS).Original Medicare
You may add a Medicare supplement plan, a standalone Part D plan, or both to Original Medicare (Parts A & B).
Medicare Supplement Plans are mostly designed to cover the portion of the cost that is left behind by Original Medicare parts A & B.
Medicare Supplements have a monthly premium and typically increase a few percent each year as we age.
Typically, Medicare supplements do not have provider networks like Medicare Advantage plans, allowing beneficiaries to see doctors who participate in Medicare across the country without a referral. These types of plans allow for more flexibility in seeing providers.
Medicare supplements do not offer prescription drug coverage, which may require one to be purchased.
There are a variety of different plans available, and some will cover more than others.
Original Medicare (Parts A and B) does not cover prescription drugs. Many people who choose Original Medicare add a prescription drug plan (Part D) or choose a Medicare Advantage plan that includes Part D. Medicare Part D plans are required to cover certain common types of drugs, but each plan may choose which specific drugs it covers.
Parts A + B Parts A + B plus Part D prescription coverage Parts A + B plus a Medicare supplement plan Parts A + B plus both Part D prescription coverage and a Medicare supplement planMedicare Advantage
Advantage plans are privately managed healthcare plans that combine Medicare Part A and B, and in some cases include Part D (prescription drug coverage). Consider it an “all in one” plan. A common question we get is “why would I want a private insurance company to manage my Medicare benefits?” The answer is simple. Medicare Advantage plan carriers are required to provide you equal or better coverage than traditional Medicare. What that means is that you get all the benefits of your Part A hospitalization coverage and all the benefits of your Part B general healthcare coverage, with (in most cases) prescription drug coverage (Part D). In addition, some plans provide coverage for dental, vision, holistic healthcare, gym memberships, and more!
Typically, there is no additional expense for selecting a Medicare Advantage plan above your required Plan B monthly premium! Normally, this monthly fee is far less than you would spend by purchasing a Medicare Supplement plan. You then only pay the applicable copay(s) for the services you use.
Medicare and many Medicare plans are a fixed amount that you pay on a monthly basis for your coverage – also known as premiums.
You also pay a portion of the cost for health care services you receive. There are three types of payments you may have:
Deductible: A set amount you pay out of pocket for covered services each year before Medicare or your plans begins to pay. Copay: A fixed amount you pay at the time you receive a covered service. For example, you might pay $20 when you visit the doctor or $12 when you fill a prescription. Co-Insurance: A percentage of the cost for a covered service that you pay when you receive it. For example, Medicare might pay 80% of the covered service and the remaining 20% would be paid by you.When can I enroll?
Your Initial Enrollment Period (or IEP) is a seven-month period of time. It begins three months before the month of your 65th birthday, the month of your birthday, and three months after your birthday month.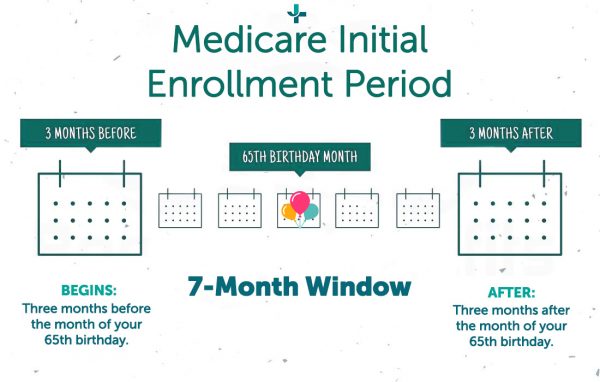
If you do not sign up during this 7-month period (unless you have other creditable coverage) you will need to wait and enroll from January 1 to March 31th for a July 1st effective date.
This is called General Enrollment Period.

Plans can change: networks, doctors, pharmacies and medication formally and tiers of medication can change.

Did you know that if you’re unhappy with your Medicare Advantage Plan (Medicare Part C), you have options? Each year, there is the Medicare Advantage Open Enrollment Period from January 1 – March 31. During this time, if you’re in a Medicare Advantage Plan and want to change your health plan, you can do one of these once during this time period:
- Switch to a different Medicare Advantage Plan with or without drug coverage.
- Go back to Original Medicare and, if needed, also join a Medicare Prescription Drug Plan.
- Permanently move out of plans service area
- Lose creditable medical or prescription drug coverage
- Move into, reside in or leave a long-term care facility
- Have Medicaid or AHCCCS in AZ or are in a Medicare Savings Programs
- Have other exceptional circumstances
You typically have a certain period of time usually 2 months from the date of the event.
There’s a lot to consider when choosing your Medicare Coverage. Jeffery Insurance will carefully walk through the right questions to make sure you are on the best plan for your needs.

